If you are a one-celled animal, life is pretty simple …
Your entire body is in contact with the environment at all times. You can grab oxygen and nutrients at will. It is sort of like being accidentally locked in Albertson’s overnight. Face it, you’re not exactly going to starve in there. (Look for me in the Bakery section).
But when we made the jump to multi-cellular (many celled) forms of life, things got more complicated. Now we have an outside and an inside. We have cells, like the ones in your liver or kidney, which are far from the outside world. They need UPS or FedEx to bring them oxygen and nutrients. Our circulatory system—the vast network of arteries and veins that travels throughout the body—is analogous to the highways and roads that allow us to drive to the supermarket or have our trash picked up every week. And if the arteries, veins, and capillaries are the roadways, then blood is the flow of traffic carrying all sorts of needed items to the cells (like oxygen) and carrying away waste products (like carbon dioxide).
But what is blood? Well, blood is mostly a mixture of two things. The first is red blood cells, which make up one-third to one-half the volume of blood, and the other component is serum which is a golden-yellow colored liquid full of everything else we need, such as sugar, salt, cholesterol, hormones, potassium, and—of course—the medicines I prescribe.
White blood cells make up a tiny portion of blood. There is one white blood cell for every 500-1000 red, so we can pretty much ignore them for these purposes. If you take a sample of someone’s blood and put it in a test tube (adding a little material to keep the blood from clotting) and wait, the red cells will fall to the bottom and the liquid component (the serum) will rise to the top. To speed things up, the blood sample is put in a centrifuge and this creates the equivalent of a high gravity situation. The red cells are pulled to the bottom in a few minutes.
Once you spin down the blood, it is easy to see the percentage of the total which is red blood cells and the percentage that is serum [see diagram]. The word hematocrit (HCT) is a medical term which just means the percentage of the total volume of blood which is red blood cells, as opposed to serum. Typically a normal hematocrit is 40%, meaning that if the tube is filled to the one inch mark with blood and you spin it down (or just let the red cells settle to the bottom) then about 4/10 of an inch will be red cells and the rest above it the watery serum.
Red blood cells have a lifespan in the body of about 120 days. They have to squeeze through very tight spaces and they tend to wear out. When they are beat up and worn, they are filtered in the spleen and broken down. The bone marrow (the space inside of bones, which are hollow, by the way) is where red blood cells are manufactured. It is funny to think that your leg bone, which has the important job of making sure you can walk, actually has a completely different business going on inside of manufacturing red and white blood cells. It is sort of like going to Home Depot and finding a dentist practicing on aisle eight.
If your body does not manufacture enough red blood cells to keep up with their aging and destruction, then you develop anemia. The hematocrit falls and the circulating blood has proportionately more of the watery serum and fewer red blood cells. If the hematocrit is 30-35%, we consider the anemia to be mild, 23-29% is moderate, and anything below that is severe.
What are the consequences of anemia? Well, the main job of red blood cells is to carry oxygen to the tissues. Fewer red blood cells means less oxygen delivery. If you’re sitting at your desk eating doughnuts, you might not notice the difference. But your exercise tolerance is going to be less, and if your anemia worsens, you are going to feel weak and tired and look pale to your friends.
There are many causes of anemia, but the most common is iron deficiency. In order to transport oxygen to the tissues, red blood cells just don’t throw oxygen willy-nilly inside themselves, like a duffel bag. Instead, red blood cells are full of a special protein which binds to oxygen and carries it to the tissues. That special protein is called hemoglobin. The word “heme” means iron and is a reference to the fact that this oxygen carrying protein, hemoglobin, has a hunk of iron in the middle. Most proteins in the body do not have metal floating in there. I sometimes think iron was an unwise choice for so critical a function. It is poorly absorbed from the intestines and is missing from many foods. Why depend on iron for so critical a task? Why not use something else? Actually, there are good reasons to use iron for this purpose.
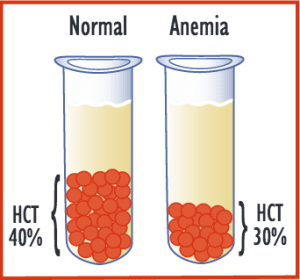
In a normal patient, red blood cells make up 40% of the volume of blood. In someone with anemia, the blood is “watered down” and red blood cells might make up 30% or less.
In any event, the most common cause of iron deficiency is the slow loss of blood. Perhaps you have heavy menstrual periods, an ulcer that bleeds from time to time, or poor shaving technique (kidding about this one, jeez). At first, no big deal, you just step up production of red blood cells. It is not the loss of red blood cells that is a problem—it’s the lost iron. Iron is poorly absorbed from the gut and you are not likely to be replacing the needed iron from dietary sources fast enough.
When your body is short on iron, it builds red blood cells smaller in size than normal. Even if I don’t run tests to measure the level of iron in the body, if I see an anemia and the lab report says the red blood cells are smaller than typical, I will usually suspect that the problem is iron deficiency. If you have an obvious reason for losing iron (heavy menstrual periods for example) then we can just confirm that the body iron levels are low and have you take a little extra oral iron to try and replace it. But if there is no obvious reason for low iron, then we look to see if you are losing iron in the stool from bleeding somewhere in the gastrointestinal system, like an ulcer for example.
If you lose a lot of blood quickly, such as in a car accident, then you have an anemia due to sudden blood loss. If your survive the accident, your body will make new red blood cells over several weeks to replace the lost ones, provided you have enough extra iron stored on hand.
There are many other causes of anemia. If you run out of vitamin B12, you can develop an anemia because vitamin B12 is needed to produce red blood cells. Alcohol can poison the production of red cells and cause an anemia. Finally, if your kidneys fail, they stop producing a hormone called erythropoietin (or EPO) which is responsible for triggering red blood cell production in the bone marrow.
One fascinating cause of anemia which shares features in common with iron deficiency and the anemia of kidney failure is the anemia of chronic disease. We’ve found that patients with certain chronic medical problems, like rheumatoid arthritis, AIDS, or certain cancers develop an anemia. Although the red blood cells are often normal in size, sometimes they are small, just like in iron deficiency. Also, the level of erythropoietin can be low, just like in kidney failure.
Why would the body, already suffering from a disease like rheumatoid arthritis or AIDS, develop an anemia? It is not because of the disease process. The body is doing it to itself on purpose.
If you don’t make enough red blood cells to
keep up with their natural aging and loss,
you develop anemia.
It turns out that we aren’t the only ones who like having iron around. Bacteria also require iron for many of their life processes. When inflammation is present, the body can’t always exactly tell the difference between rheumatoid arthritis, cancer, or an infection. It takes the safe route and bets on infection. After all, through much of our evolutionary history, infections were the big thing that killed us. So if the body thinks it is chronically “infected” it hides the iron. It takes the iron away from the bone marrow and sequesters it in a group of cells distributed throughout the body called the reticuloendothelial system, cells which function as garbage collectors. The body also lowers the level of erythropoietin. These changes hide the available iron and reduce the circulating red blood cells. It provides a small amount of protection against infection. It is a classic “poison pill” defense. This explains our body’s love/hate relationship with iron. We like it, but bacteria like it, too. This may be why iron is poorly absorbed from the intestine and why many people run chronically low on iron.
We can defeat this self-defense mechanism in the anemia of chronic disease by giving patients iron orally and erythropoietin by injection. Patients will feel better, but their risk of serious infections also goes up somewhat because bacteria like that iron just as much as we do.
When patients feel weak and tired, they worry about anemia. A simple blood test can tell us if anemia is present, and further studies can usually find out why.